Lancet Global Health Blog - Non-doctor emergency surgeons are saving thousands of lives in rural Ethiopian hospitals

Dr. Biku Ghosh, OBE, FRCS, Founder and former Chair, Wales for Africa Health Links Network and Co-founder of Southern Ethiopia Gwent Healthcare Link

Dr. Aberra A Gobeze, MD, Assistant Professor of Urology and Surgery, Hawassa University Referral Hospital, Hawassa, Ethiopia, and Co-founder of the Southern Ethiopia Gwent Health Care Link
The Lancet Global Health Blog appears to be offline and therefore, the original article is reproduced here.
At the end of the first long day of advanced skills training in emergency surgery and obstetrics, Murida Shamil approached me timidly. She was 28 years old and had travelled nearly a day and a half by public transport from her rural primary hospital to Awassa to attend this course.
“Dr Biku I am sorry that I have been late each time during the coffee and lunch breaks to return for the skills training and you all had to wait. Sorry I had to breastfeed my 6 month old daughter. My husband who was looking after her in between was late. I have told him off.”
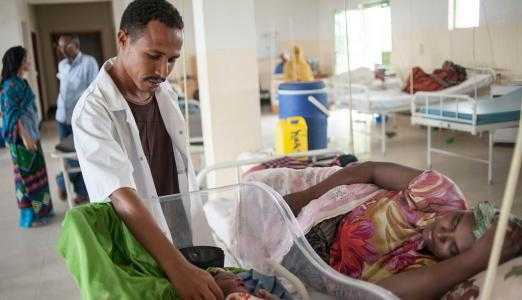
Our Southern Ethiopia Gwent Health Care Link was the first to introduce Continuing Medical Education (CME) programmes in emergency surgical and obstetric training for non-doctor health officers in the Southern Nations, Nationalities, and Peoples’ Region (SNNPR) of Ethiopia in 2000. By the end of 2005, after consultation between our organisation, THET, the Federal Ministry of Health in Ethiopia, WHO, Addis Ababa University representatives, and the British Embassy (which was at that time funding our CME programme), consensus was reached on starting a task force in the country to develop a Masters programme in emergency surgery and obstetrics. The task force involved all the then-existing five medical universities as well as representation from other bodies.
The Masters programme was rolled out in 2009. The strategy was intended to overcome the human resource scarcity of trained surgeons within a short period of time especially in rural Ethiopian hospitals. Trained health officers and BSc nurses who have been working in health facilities for a minimum of 2 years are recruited through a tough entrance examination. They are then trained in a 3-year special MSc course designed for producing emergency surgical officers competent to perform emergency surgical, gynaecological, and obstetric operations such as caesarean sections.
This Integrated Emergency Surgical Officer (IESO) training programme started in three universities with an intake of 43 students and has since been expanded to 11 universities. The first batch of graduates qualified in 2012/13. Currently there are 153 qualified IESOs deployed in different regions. By the end of 2015 the initiative plans to train 800. The future plan is to make one IESO available per 100,000 population throughout the country.
The Ethiopian Government has recently undertaken a massive hospital-building programme throughout the country. In the SNNPR, with a current population of nearly 26 million, the number of hospitals has increased from only 14 in 2001 to more than 50 in 2015. Only 26 of these hospitals are currenly carrying out emergency medical or obstetric surgery, with only 44 trained surgeons, only 11 of whom are medically qualified surgeons or gynaecologists; the other 33 are IESOs. Many of these hospitals only have IESOs. With the help of the SNNPR health authority, we were keen to establish what impact the IESOs are having in the region and support them with further training.
A UK team of one general surgeon (myself), two orthopaedic surgeons, and two anaesthetists, with the help of another surgeon and two gynaecologists from Awassa teaching hospital, arranged a 5-day advanced skills course in early November, 2015. All 33 IESOs in SNNPR hospitals were invited. Only 24 of them could attend; five had only qualified that year. Between them, these 24 IESOs have carried out about 4856 caesarean sections, operated on 562 ruptured uteruses, and done 1366 laparotomies for various other indications. Thus potentially more than 6000 lives (plus another 4500 newborn lives) have been saved by these IESOs in the past 3 years alone.
Murida graduated as an IESO just over 3 years back. Since then she has carried out 400 successful caesarean sections, dealt with 64 ruptured uteruses (with only one death), and done approximately 200 laparotomies for various indications. And she also managed to have her first baby daughter!
We were all extremely impressed by the technical skills of these young IESO during this course and have no doubt that they will continue to save many thousands lives in rural hospitals in Ethiopia for years to come. Is there a lesson for other countries to learn from this?
This is a joint post with Dr. Aberra A Gobeze, MD, Assistant Professor of Urology and Surgery, Hawassa University Referral Hospital, Hawassa, Ethiopia, and Founder of the Southern Ethiopia Gwent Health Care Link.